Contact Vicki
If you have any questions or would just like more information please don't hesitate to get in touch by clicking the button below and filling out the contact form.
Contact Vicki
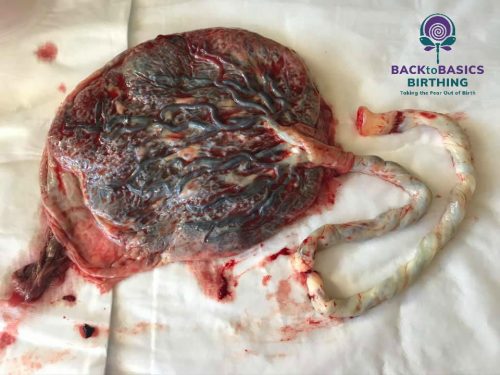
Have you given any thought to birthing your placenta? Yes, that’s right, after your baby is born it doesn’t just stop there – the placenta needs to come out too. The placenta is an incredible organ and has been the lifeline of your baby for the duration of your pregnancy and it needs to be given a lot more acknowledgement and credit than just being discarded after birth. As you’ve probably guessed, I’m a big fan of the placenta and the umbilical cord.
Without the placenta, there can be no new life.
Your baby uses the placenta as it’s lungs, digestive system and liver.
Even though your baby doesn’t breathe inutero, there is a large vein in the umbilical cord that carries the oxygen filled blood from the mother to the baby via the placenta, and there are two smaller arteries in the umbilical cord, which carry oxygen depleted blood and waste back to the mother via the placenta.
The cord is filled with a jelly like substance called Wharton’s Jelly that protects the vein and two arteries from being compressed during baby movements, labour and birth.
This is why it is rare for a baby with the cord wrapped around its neck to need a caesarean birth, because the baby is not breathing through its respiratory system.
This is also why babies can be born underwater and the head may be sitting there under water for some time before the rest of the body is born and then lifted up out of the water, where the cold air hits the baby’s face and triggers the first breath, which activates the respiratory system.
After birth when your baby takes its first breath, blood is shunted to the lungs and the two arteries constrict to stop the flow of blood and the vein collapses.
The vein and arteries then close and become ligaments – the ones closer to the belly button serve no purpose, but the more internal parts become part of the circulatory system.
So, once the baby is born, the next stage is to birth the placenta.
If the mother chooses to have a physiological birth of the placenta, this means that she waits for her contractions to start again to detach the placenta from the uterine wall and be born.
It is hard to predict how long this process can take, sometimes it is as quick as 15 minutes and then other times it can be over an hour or longer. If the mother has skin to skin and also waits for baby to breast crawl or puts her baby straight to her breast to start sucking, nuzzling or just touching the breast, this will then trigger the release of more oxytocin to increase the effectiveness of contractions to birth the placenta.
We want that smell, touch, taste, sound and breast to trigger the release of more oxytocin.
We also encourage the mother to “wait for white” where the blood has drained out of the placenta through to baby and the umbilical cord has turned white.
This means the placenta is empty and less bulky and can exit more easily.
The contractions will start up again but usually not as intense, and sometimes mums don’t even notice as they are too caught up having skin to skin and bonding with their baby and enjoying those moments of becoming a newborn mother. These contractions will help the placenta to gradually dislodge from the wall of the uterus and it is important for care providers to just be patient to wait for that to happen.
During those contractions, the muscle fibres of the uterus retract and constrict the blood vessels supplying the placenta. The veins then rupture, and the villi breaks away from the uterine wall.
A clot forms behind the placenta and the placenta site is quickly covered by a fibrin mesh.
The placenta and the membranes will drop to the bottom of the uterus and out through the vagina.
The midwife will examine the placenta and membranes to make sure that nothing has been left behind.
She will also feel the mums’ uterus by pressing down through the abdomen to check that the uterus is contracting hard to stop the bleeding from the place where the placenta was attached.
This may be extremely uncomfortable for mums, so it is important that women are aware that this may happen so that they are prepared for this and to know they can tell the midwife to stop if it becomes too distressing or painful.
I always encourage mums to have a look at the placenta as it is a wonderful organ that has been her baby’s lifeline through her pregnancy.
Dr Rachel Reed from Midwife Thinking states that the birth of the placenta and haemostasis, which is the prevention of excessive blood loss, and relies on effective uterine contractions.
Ineffective uterine contractions is the main cause of post-partum haemorrhage.
She says there are two main causes of ineffective uterine contractions after birth to prevent the placenta being born.
These are:
1. Hormonal – there is not enough oxytocin due to an overload of syntocinon during labour to induce or augment the labour, and
2. Mechanical – something is in the way and usually that is a full bladder taking up space and stopping the uterus from contracting.
This is where mums should be encouraged to get up and move around or sit on the toilet, and the midwife can put a pan in the toilet to capture the placenta if it falls out while on the toilet.
If the placenta doesn’t come out, then it will be suggested that the mum have an actively managed placenta with an injection of syntocinon to help the placenta out.
A managed third stage means that the mother is given an injection of syntocinon (synthetic oxytocin) in her thigh or buttock along with cord traction (pulling on the cord) to speed up the process.
I suggest that if you decide to have the injection then ask for it to be given after the cord has stopped pulsating and has been clamped, which prevents the syntocinon going through to the baby.
Some hospitals still routinely administer the syntocinon injection to reduce the risk of a post-partum haemorrhage, so it is important to ask your care providers questions about what their procedures are, and to have in your birth plan if you want to have a physiological birth of the placenta or an actively managed one or a “wait and see” approach.
You can always change your mind if there is excessive bleeding and then you can consent to the injection if it is needed.
However, if you have had a “medical birth” rather than a “physiological birth” then it make sense to have active management of the placenta, because all the rhythm and flow of natural hormones has been interrupted.
Dr Rachel Reed discusses the interruption of the normal physiological process, which can then interfere with the release of the placenta, which would inevitably mean the requirement for active management to prevent a post-partum haemorrhage.
The summary of this article:
“Active management of the placenta will reduce the chance of a PPH in a setting that does not support physiology and in which routine intervention is the norm. There are further options within active management that can be negotiated. Physiological placental birth is an option, and possible if you manage to avoid induction, augmentation, an epidural or complications – but be aware of how difficult it may be, and don’t beat yourself up if it doesn’t happen.”
To read the full article CLICK HERE
Dr Rachel Reed has also written a book called “Why Induction Matters” which outlines how drugs and interventions can interfere with the normal, physiological process and I definitely recommend all pregnant women get a copy and have a read.
I also challenge medical care providers to read this book and look at what you do, and perhaps consider doing things in a different way and the reasons why.
Dr Sarah Buckley even suggests that due to the medical management of the third stage, this may even lead to many of the problems that active management is meant to avoid.
In her article she states:
“During the third stage of labour, strong uterine contractions continue at regular intervals, under the continuing influence of oxytocin. The uterine muscle fibres shorten, or retract, with each contraction, leading to a gradual decrease in the size of the uterus, which helps to shear the placenta away from its attachment site on the mother’s uterine wall. Third stage is complete when the mother births her baby’s placenta.
For the new mother, the third stage is a time of reaping the rewards of her labour. Mother Nature provides peak levels of oxytocin, the hormone of love, and endorphins, which stimulate the brain’s reward and pleasure for both mother and baby.
Skin-to-skin contact and the baby’s first attempts to breast feed further increase maternal oxytocin levels, strengthening the uterine contractions that will help the placenta to separate, and the uterus to contract down.
In this way, oxytocin acts to prevent haemorrhage, as well as to establish, in concert with the other hormones, the close bond that will ensure a mother’s care and protection, and thus her baby’s survival.
Please read the full article by Sarah, because it is so important that you understand that hormonal physiological process.
To read the full article CLICK HERE
I highly recommend that you also get a copy of Sarah Buckley’s book called Gentle Birth, Gentle Mothering – it is the one book that I say every pregnant woman should read, not only for pregnancy but for the postpartum period as well.
We have lost so much of this instinctual behavior when it comes to labour and birth.
We need to go back to basics and find the missing links.
We need our care providers to not just train in the medical, pathological side of birth, but also the instinctual and primal connection of birth, but even more importantly, the mother / baby connection.
Mother and baby working together to birth in a positive, calm way.
If you have any questions or would just like more information please don't hesitate to get in touch by clicking the button below and filling out the contact form.
Contact Vicki