Contact Vicki
If you have any questions or would just like more information please don't hesitate to get in touch by clicking the button below and filling out the contact form.
Contact Vicki
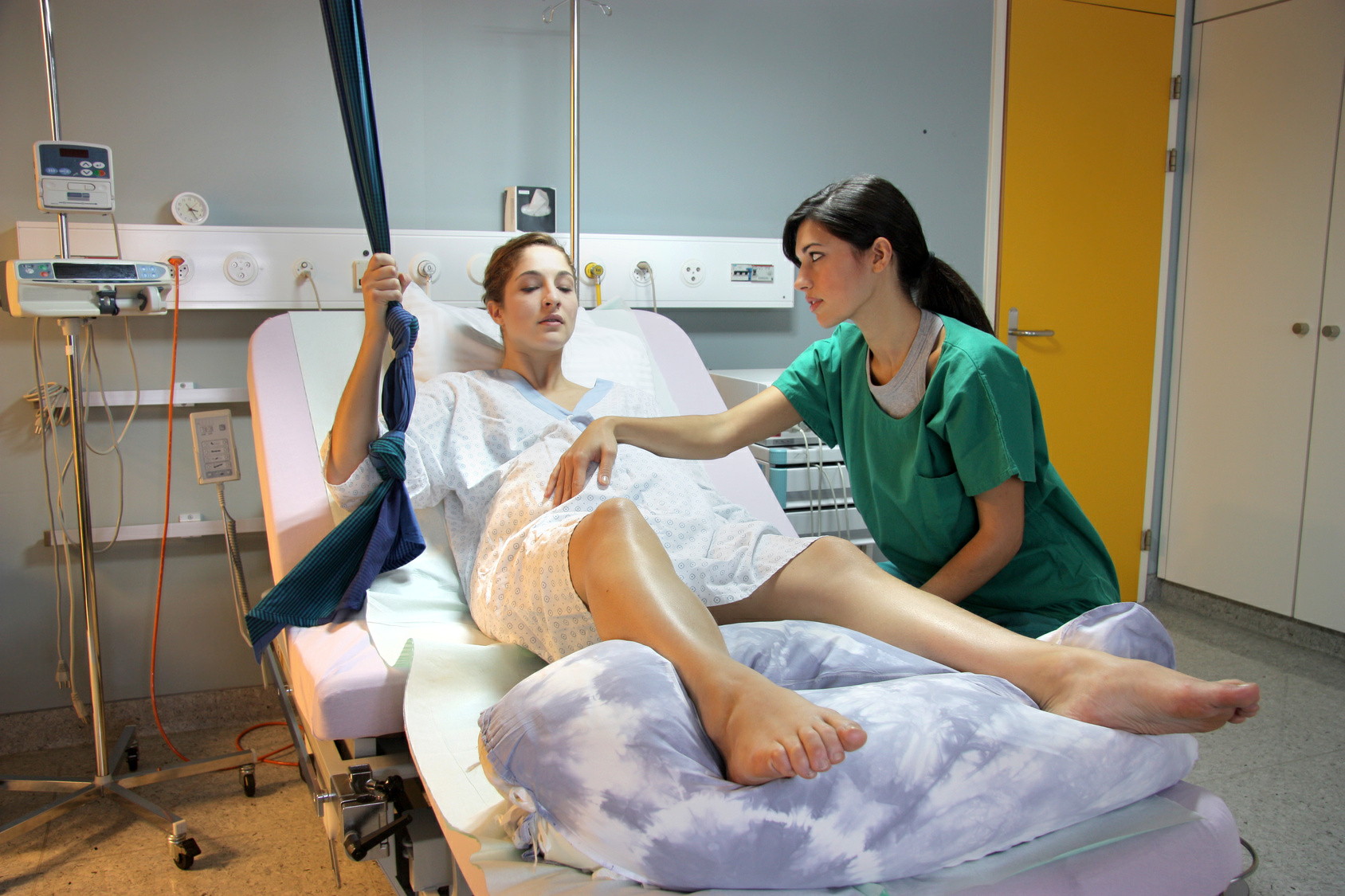
One of the main concerns women have about their labour and birth will be whether or not they will be able to cope with the intensity of pain. Here are some medical pain relief options for labouring women to give you a starting point of what is available, but also what you need to do more research on so you understand all the risks and benefits.
If women have fear about pain, this will create tension in the muscles and restrict oxygen flow that will create or intensify the level of pain they experience. My first suggestion would be to do either my Back to Basics Birthing classes or Hypnobirthing Class or my Online Course to help you with tools and techniques for releasing fear, creating confidence and having a knowledgeable and supportive partner there with you.
Obviously, women need to decide what is going to be best for them in terms of medical pain relief and intervention options. When you do my classes, my role is to provide you with enough information so that you work through your fear of labour and birth so the need for medical intervention is reduced or even eliminated – however, like anything when it comes to you and your body, you do have a choice.
There are two main groups for pain relief, the first being medical to reduce or eliminate pain and the second is more natural, non-medical options.
My catch phrase has always been that with choice comes responsibility and consequences, which can be positive or negative.
Here is something for you to contemplate:
During your entire pregnancy did you stop drinking alcohol? Did you stop eating certain foods which you thought may have caused harm to your baby? If you were a smoker did you stop smoking? Did you stop doing anything that you thought might harm your baby in any way, shape or form?
If you answered yes to these questions, then you need to also research the effects that using drugs in labour will have on you, your baby and your postpartum period.
Here are a few of the pain relief options that are offered to women during labour and in my next blog we can look at some of the natural pain relief options available to you:
There are no studies around the use of paracetamol during early labour.
There seems to be some suggestions that women who are taking paracetamol during early labour are having longer labours.
There seems to have been a shift in the latent phase of labour since the 1980’s and 1990’s where they are becoming longer and more difficult.
This seems to coincide with the introduction of paracetamol.
What we do know from the drug studies is that paracetamol is known to be an inhibitor of prostaglandin synthesis.
Women need to be producing prostaglandins to ripen the cervix and the initiation of smooth muscle uterine activity in early labour.
Some more information from the Undercover Midwife CLICK HERE
This looks like a medical device, but it is actually a natural, drug free option for pain relief.
TENS stands for Transcutaneous Electrical Nerve Stimulation.
A maternity TENS machine consists of a battery-powered, hand-held controller connected by fine leads to four flat pads.
The pads are covered in a firm gel that helps them stick to your back.
The machine sends small, safe pulses of electrical current via the leads to the pads on your skin.
The pulses pass through your skin and into your muscles and tissues.
This gives you a gentle tingling or buzzing sensation, which may be stronger or weaker, depending on the setting level.
For labour the best TENS is the Obstetric TENS because it also has a “boost” button that the woman presses during a contraction that sends a constant impulse, which offers a lot more relief, and once the surge has stopped the woman then chooses the normal setting again where it then sends a pulsing sensation, which helps to relax the muscles.
I have seen a lot of women saying on social media that they used the TENS machine, but it didn’t work for them, but upon questioning them I find they didn’t put the TENS machine on early enough. The problem is that women put them on too late. They wait until they start getting really intense contractions and then put the pads on and this is too late. The idea of the TENS machine is to start releasing endorphins into the body so that by the time you do have intense surges you already have a build-up of endorphins to manage this.
Only limited research is available on the effectiveness of the TENS machine, and we don’t really know exactly how the TENS works to help you cope in labour, however it’s probably due to a combination of factors such as:
Here is what the Cochrane Review said:
“There is only limited evidence that TENS reduces pain in labour and it does not seem to have any impact (either positive or negative) on other outcomes for mothers or babies. The use of TENS at home in early labour has not been evaluated. TENS is widely available in hospital settings and women should have the choice of using it in labour.”
WHAT’S THE RESEARCH – CLICK HERE
The TENS machine that I love and recommend to my clients is the Elle TENS Australia Obi-Tens as it is the basic model and simple to use. Alternatively, ask in one of the pregnancy or mums groups on Facebook. I have picked up some bargains from women wanting to sell them and they could be brand new for a fraction of the cost.
Nitrous Oxide (also referred to as “the gas”) is a combination of oxygen and gas.
Women will use a mouth piece with a tube connected to the gas bottle to breathe in the gas to the lungs.
It then enters the blood stream and to the brain within 15 seconds and can provide pain relief for a short period of time.
Once you stop breathing the nitrous oxide and breathe air this causes the gas to wear off.
Nitrous Oxide does pass the placenta to the baby, however does not affect the baby like opiates would as it again is quickly metabolised in the baby’s body.
The gas may be beneficial to some women and then totally useless for others.
Some additional information can be found at this link:
Nitrous Oxide – Clinical Implications – CLICK HERE
Sterile water injections were first mentioned back in 1885 when Dr. William Halsted wrote: “the skin can be completely anesthetized to any extent by cutaneous injections of water.”
Injections of sterile water into four spots just under the skin over the sacrum have now started to be offered as pain relief for back pain in some hospitals around Australia.
There is not a great deal of research or evidence on this method of pain relief and there has been varied feedback from women who have used this form of pain relief.
Sterile water injections provide effective back pain relief (as opposed to pain relief from contractions) and can last anywhere from 45 minutes up to two hours and can be repeated.
The injections are usually administered by two midwives during a contraction.
There have not been any recorded side-effects to having sterile water injections other than a burning / stinging sensation upon injection at the site lasting for a few seconds.
As the pain in the back subsides and the muscles relax this may assist in progressing labour and help a woman to cope better through her contractions.
What’s the evidence on using Sterile Water Injections – CLICK HERE
Morphine is a natural drug that is derived from the opium poppy.
Pethidine is a narcotic drug (opioid) that is synthetically made, like heroin.
They both work to mimic your body’s own endorphins; however, they are highly addictive (although this will not occur with the limited use during labour).
They are both administered into the thigh or buttock via injection by your midwife and does not need to be monitored by an anaesthetist. It usually takes around ten to twenty minutes to take effect and can last up to three hours.
WANT TO KNOW MORE – CLICK HERE
An EPIDURAL CATHETER is where a needle is fixed to a thin catheter tube and inserted into the spinal cord between the vertebrae that goes into the epidural space. This can be done at any time during active labour up until full dilation of the cervix.
The catheter tube is then left in and connected to a pump where you receive an infusion of numbing medication for as long as labour lasts, and you control the administration of the drug with a hand-held pump. This is regional analgesia, so it works on the pelvic area to provide pain relief as opposed to anaesthesia, which blocks sensations completely.
The dosage is set by the anaesthetist and you will have to wait for the pump to let you know when you can administer the next dose. Depending on the dosage you may still be able to feel sensations, but the intensity of pain has been dramatically reduced, so this can be a really good option for women so they are still able to be active.
There are now “Walking Epidurals” which allow you to be more mobile while in labour. Usually you can’t go walking because your strength and mobility is still affected and you will be attached to the foetal monitoring machine unless you have the telemetry (wireless) monitoring but you can feel your legs and all the sensations.
Use a peanut ball and ask your midwife to help you change positions on the bed, or to get up kneeling and leaning over the top of the bed so you are using gravity to bring baby down and don’t let anyone tell you that this can’t be done.
A SPINAL BLOCK epidural is where a woman needs to have a caesarean or pain relief needs to take effect very quickly and makes you numb so you don’t feel anything for up to two hours. Narcotics or anaesthetic (usually Bupivacaine or Lidocaine) is injected once with a needle directly into the spinal fluid.
More on Spinal Blocks – CLICK HERE
If you have an epidural it is hospital policy for you and your baby to have constant foetal monitoring (CFM) to ensure that you are both safe once the drug takes effect.
Some hospitals don’t allow women to get off the bed at all when an epidural is in because of litigation reasons (e.g. falling over and injuring yourself).
More on Epidurals
Sarah Buckley on Epidurals
Different Epidurals
Always use your BRAIN to ask all the right questions, to get all the answers you need to make an informed choice.
So you would ask your care provider about the:
BENEFITS – why is this going to be a positive choice?
RISKS – what risks are involved with choosing this option?
ALTERNATIVES – can I do something different that is more natural?
INSTINCTS – how do you feel about this option – what does your gut tell you?
NOTHING – what if you just wait a bit longer?
But also ask yourself these questions – because your answers may be different subconsciously so ask yourself and see what comes up – and if you are unsure, then just wait and see.
Check out some of the natural pain relief methods you can use to try and avoid drugs. Remember though, there is a difference between managing pain and suffering, so if you feel that your birth will be far better for you by using some form of medication then you can make that decision based on your needs, not what someone else wants you to do.
If you wish to use natural forms of pain medication, put this in your birth plan to ensure that your care providers are not constantly asking you if you need drugs – tell them you will ask for it if you need it. Start off with the natural methods first and then if you need something more you can systematically work your way through the list of options that are available to you.
This is just a brief outline of pain medication, and I do encourage you to do more research on these options, so you understand all the benefits and risks.
Would you like to learn how to manage your labour and birth without drugs or medications?
My classes are a great way to prepare and feel confident about your birth.
My name is Vicki Hobbs, and I am a Childbirth Educator (Back to Basics Birthing), Hypnobirthing Practitioner, Certified VBAC Educator, Remedial Massage Therapist specialising in Pregnancy & Postpartum Massage, Birth & Postpartum Doula, Certified Placenta Encapsulator, Hypnotherapist, Aromatherapist, Reiki Practitioner and Life Coach. I am a serial workshopper and learner, so that I keep up to date with new research and information so that I can provide you with up-to-date resources. My focus has always been on the mind, the body and the emotions and how they all need to be in balance for harmony. You can subscribe to my newsletter by adding your details in the box on the right-hand side and when you do, I will send you a free relaxation meditation to help you feel calm and relaxed. I am based in the northern suburbs of Perth and can be contacted by email at [email protected] or go back to my Blog Page for more great articles and information.
If you have any questions or would just like more information please don't hesitate to get in touch by clicking the button below and filling out the contact form.
Contact Vicki